What is a stress fracture?
Stress fractures are small cracks or breaks in otherwise healthy bone, typically related to overuse and related to repeated impact on the bone. They mainly occur in weight bearing bones – typically the shin and foot.
Stress fractures are ‘fatigue-induced’ fractures due to repetitive stress over time rather than a one-off event. Stress fractures were first described in 1855 in Prussian soldiers’ feet and named ‘march fractures’.
40years later with the invention of X-rays their characteristics were confirmed. In 1958 the first report of stress fractures in athletes (in the shin bone) was made.
Stress fractures are relatively uncommon in the general population with occurrence of less than 1%. Often runners or people who take part in repetitive impact sport are affected, especially if they have increased their training load/volume abruptly. The cause of a stress fracture is often multifactorial and can require input from different specialists to optimise healing and prevent recurrence.
Symptoms typically begin with pain over the effected area that develops over a few weeks. Pain is generally worse on weight bearing and relieved by rest. The bone involved is often painful to touch and there can be associated swelling. As symptoms worsen sometimes pain at night sometimes becomes apparent.
How does a stress fracture happen?
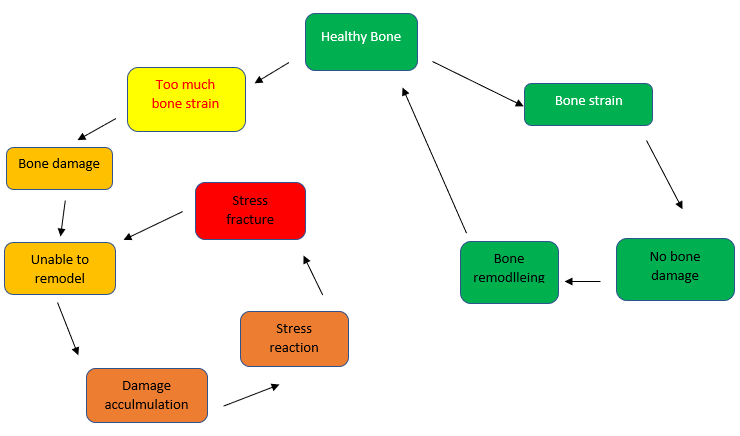
Bone is a living tissue and is constantly going through a process of ‘bone remodelling’ – older/damaged bone is removed by special bone cells called ‘osteoclasts’ and is replaced by new healthy strong bone by another type of bone cell called ‘osteoblasts’. This process is what allows bone to adapt as we put it through different types of stress, strains and loading activity.
Bone stress occurs when this process becomes imbalanced and bone is unable to adapt fast enough to new loads and causes an area of weakness. This area of stress can develop into a stress fracture if the amount of load of the bone is not reduced. Stress fractures normally occur when there is a sudden increased change in activity or training load (e.g. reducing recovery time between training sessions, increasing training frequency, increasing training intensity/volume) without enough rest time for the bone to adapt and remodel.
Stress fractures normally occur in weightbearing bones as loading is a main factor. Most common sites are the shin and foot, but they can sometimes occur in the hip, pelvis or back.
A stress fracture is sometimes called an insufficiency fracture – this is when it has happened after ‘normal’ stresses have been applied to a bone that is deficient in its ability to tolerate such load. This is often due to conditions that affect bone strength/health such as osteoporosis (reduced bone density), Coeliacs disease, Crohns disease, vitamin D deficiency, hormonal abnormalities and the use of oral steroid medication (not steroid topical gels or nasal sprays).
How are stress fractures diagnosed?
Often diagnosis is made by x-ray but sometimes even if an x-ray is normal and there are clinical concerns then further imaging (like an MRI scan) is needed. Once diagnosis has been made you should be referred to your local Sports Medicine department (e.g. Nuffield Orthopaedic Hospital’s OxSport Clinic).
How are stress fractures managed?
It is very important that the bone is allowed to heel – this normally involves a relative reduction of weight bearing. This may mean just rest from your sporting activity or it may mean using crutches and not putting any weight at all on the affected leg. It depends on the type, severity and location of the stress fracture and the individual’s activity levels. The amount of time the reduction of loading needs to continue for also varies from patient to patient and is guided by the expert clinician whose care you are under. Most people will get back to their sport within 10-16 weeks. Rehabilitation normally starts with non-weight bearing exercises and then a gradual increase in weight bearing and strengthening exercises, followed lastly with a phased return to impact and sport.
It is very important that the bone is allowed to heel – this normally involves a relative reduction of weight bearing. This may mean just rest from your sporting activity or it may mean using crutches and not putting any weight at all on the affected leg. It depends on the type, severity and location of the stress fracture and the individual’s activity levels. The amount of time the reduction of loading needs to continue for also varies from patient to patient and is guided by the expert clinician whose care you are under. Most people will get back to their sport within 10-16 weeks. Rehabilitation normally starts with non-weight bearing exercises and then a gradual increase in weight bearing and strengthening exercises, followed lastly with a phased return to impact and sport.
As well as managing the fracture and setting out the plan for treatment, the specialist clinic may also want to get blood tests and further scans to check your general bone health and make sure you do not have any other underlying health issues which have increased your risk of a stress fracture.
Preventing further stress fractures
Sometimes medication is needed to help with bone health and this would be advised by the specialist clinic. Other things you can do to help yourself include having a diet that will help with bone health (discuss this with your GP or a dietician). It is also wise to look at biomechanical factors/sporting techniques that may have predisposed you to increased stress going through the bone. Checking your training programme is sensible and balancing your training with other types of exercise will assist your body’s ability to cope with your chosen sport. These are all things a physiotherapist should be able to help you with.
At Flex Physiotherapy Practice we have seen many patients referred with stress fractures, and in my role as a specialist physiotherapist in the trauma clinic at the John Radcliffe Hospital I see several most months. If you have had a recent stress fracture and need physiotherapy input, or are concerned you may have one and want it assessed clinically then please get in contact. We would be happy to assess your training and biomechanics so that you can regain or maintain your ‘match fitness’ and keep you happy and healthy!
Ed Brown – Senior Physiotherapist
Flex Physiotherapy Practice